Public Health
Sex and violence may not really sell products

|
f there’s one thing advertisers think they know, it is that sex and violence sell.
A new analysis, however, provides some of the best evidence to date that this widely accepted adage just isn’t true.
Researchers analyzed the results of 53 different experiments (a so-called meta-analysis) involving nearly 8,500 people, done over 44 years. All of these experiments examined some facet of the question of whether sexual or violent media content could help sell advertised products.
When all the results are considered together, the overall conclusion, with some caveats, is that programs featuring violence and sex aren’t the ideal context for effective advertising, said Brad Bushman, co-author of the study and professor of communication and psychology at The Ohio State University.
GPs and the Fit for Work scheme

|
An editorial by primary care researchers at Plymouth University Peninsula Schools of Medicine and Dentistry, and published today, Monday 29 June 2015 in the British Journal of General Practice, analyses the GP role in the sickness certification process and the new Fit for Work scheme and suggests that GPs are key to supporting individuals to maintain the hope and belief that they can work, “rather than adding to the numbers of individuals off work on long term sickness who may have been able to work.”
The Fit for Work Scheme will be introduced in most regions in England and Wales at the end of this month. Its aim is to provide additional support for those in employment at risk of long term incapacity by using an occupational health-based assessment and a plan for helping individuals return to work.
The GP’s role in the new voluntary scheme is advisory, supporting their patients to consider the benefits of extra support. This complements the recently introduced ‘fit note’ certificate that allows GPs to be clearer about their patients’ capacity to work and extra support that may help them return to work.
Study shows global warming is unlikely to reduce winter deaths

|
A study by researchers at Columbia University’s Mailman School of Public Health debunks the assumption that global warming will lead to a decline in the number of deaths in winter. Findings by Professor Patrick Kinney, ScD, professor of Environmental Health Sciences and director of the School’s Climate and Health Program, showed that a warming climate trend led to much smaller reductions in cold-related mortality than some experts have anticipated. Among 39 cities in the U.S. and France, there was no evidence that cities having warming temperatures experienced any less winter mortality than did cooler cities.
“Some have claimed that warmer winters due to climate change will lead to big reductions in winter deaths. Our work suggests that this is unlikely to be the case,” said Dr. Kinney, who was a lead author on the recent report from the Intergovernmental Panel on Climate Change and also serves on the New York City Panel on Climate Change.
If cold temperatures were directly responsible for winter mortality rates, then we would expect future warming to lead to substantial reductions in winter mortality, according to Dr. Kinney. On the other hand, “climate warming would have little benefit if seasonal factors other than temperature are mainly responsible for winter excess mortality,” he noted.
Academies make recommendations for improving public health

|
In recent decades, enormous successes have been achieved in the field of public health. Three examples of these are the fight against HIV, the reduction in cardiovascular disease, and protection for non-smokers. For Germany to make even better use of the potential of public health, it needs more political support, improved research structures, and stronger international involvement. The German National Academy of Sciences Leopoldina, acatech - the National Academy of Science and Engineering, and the Union of the German Academies of Sciences and Humanities point this out in a joint statement entitled “Public Health in Germany - Structures, Developments and Global Challenges”, published today.
Public health is the science and practice of preventing disease, prolonging life, and improving quality of life across an entire population. The concept covers the general promotion of health via comprehensive, organised measures at all levels of society. Research questions and measures related to public health affect all sectors of the healthcare system, the education and social systems, and parts of the economy. Germany is doing outstanding research on various aspects of public health. However, the structures in research, teaching and practice are not yet optimally developed - especially considering the major international challenges that exist. In their “Public Health in Germany” statement, the academies make recommendations on how the field can be improved in Germany.
(1) The academies’ recommendations for education and further training include: improving collaboration between public health researchers, the public healthcare service, public health practitioners, and the public; coordinating professional education goals at national level; establishing interdisciplinary training schemes; opening up new career paths in public health; and incorporating elements of public health into the curricula of all medical professions. Public health professions should be made more attractive and more respected career options.
As death rates drop, nonfatal diseases and injuries take a bigger toll on health globally

|
People across the world are living longer but spending more time in ill health as rates of nonfatal diseases and injuries - including diabetes and hearing loss - decline more slowly than death rates, according to a new analysis of 301 diseases and injuries in 188 countries.
Using a measurement known as years lived with disability, or YLDs, researchers from around the world quantified the impact of health problems that impair mobility, hearing, or vision, or cause pain in some way but aren’t fatal. In 2013, low back pain and major depressive disorder were among the 10 leading causes of YLDs in every country. Other leading causes globally included neck pain, anxiety disorders, migraine headaches, and diabetes. The leading causes of years lived with disability have remained largely the same during this period, but they are taking an increased toll on health due to population growth and aging.
YLDs per person increased in 139 of 188 countries between 1990 and 2013, meaning that more people are spending more time in poor health. Musculoskeletal disorders, combined with fractures and soft tissue injuries, accounted for one-fifth of YLDs globally in 2013, ranging from 11% in Mali to 30% in South Korea. Mental and substance abuse disorders also caused 20% of YLDs globally, ranging from 15% in Germany to 37% in Qatar.
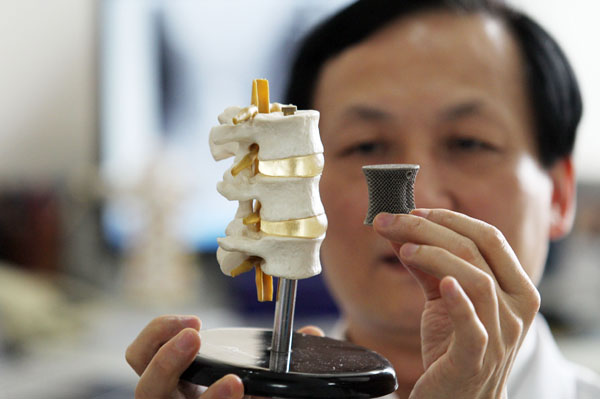
Designing better medical implants
|
Biomedical devices that can be implanted in the body for drug delivery, tissue engineering, or sensing can help improve treatment for many diseases. However, such devices are often susceptible to attack by the immune system, which can render them useless.
A team of MIT researchers has come up with a way to reduce that immune-system rejection. In a study appearing in the May 18 issue of Nature Materials, they found that the geometry of implantable devices has a significant impact on how well the body will tolerate them.
Although the researchers expected that smaller devices might be better able to evade the immune system, they discovered that larger spherical devices are actually better able to maintain their function and avoid scar-tissue buildup.
“We were surprised by how much the size and shape of an implant can affect its triggering of an immune response. What it’s made of is still an important piece of the puzzle, but it turns out if you really want to have the least amount of scar tissue you need to pick the right size and shape,” says Daniel Anderson, the Samuel A. Goldblith Associate Professor in MIT’s Department of Chemical Engineering, a member of MIT’s Koch Institute for Integrative Cancer Research and Institute for Medical Engineering and Science (IMES), and the paper’s senior author.
Single low-magnitude electric pulse successfully fights inflammation

|
The Feinstein Institute for Medical Research, the research arm of the North Shore-LIJ Health System, and SetPoint Medical Inc., a biomedical technology company, today released the results of research on the therapeutic potential of vagus nerve stimulation. In a paper published by Bioelectronic Medicine, Kevin J. Tracey, MD, and his colleagues at the Feinstein Institute, explore how low-level electrical stimulation interacts with the body’s nerves to reduce inflammation, a fundamental goal of bioelectronic medicine.
Prior to this study, it was not understood which vagus nerve fiber types were responsible for reducing the body’s inflammatory activity. The paper’s findings indicate that activation of either motor or sensory vagus nerve bundles can diminish inflammation.
“Identifying the exact role of the different nerve bundles in the inflammatory reflex bolsters our understanding of the relationship between the central nervous system and the vagus nerve,” said Dr. Kevin J. Tracey, president and CEO of the Feinstein Institute. “Furthermore, we now know that stimulating the vagus nerve for as little as half a millisecond is enough to inhibit tumor necrosis factor (TNF) production.”
After establishing the neural bundles activated in vagus nerve stimulation, the researchers found that only low-intensity, short-duration, electric pulses were needed to reduce the production of inflammation-inducing cytokines. Repetition of the pulses did not increase the success of the treatment in this experiment indicating that a single stimulating pulse is potentially sufficient.
Total annual hospital costs could be reduced by rapid candidemia identification

|
A new study describes a model that estimates the economic consequences of using the T2Candida® Panel (a novel diagnostic product that provides Candida detection) as an adjunct to the current blood culture-based diagnostic strategy in a high-risk hospital patient cohort. It estimates that a typical hospital could save as much as $5,858,448 in total annual hospital costs. The study was published online ahead of print in Future Microbiology.
Candida species are a lethal form of common bloodstream infections that cause sepsis. They are associated with high patient mortality and excess inpatient costs because growth-based detection of Candida can delay treatment decisions. Improvements in outcomes are dependent on early identification of candidemia and timely administration of appropriate antifungal therapy. The T2Candida Panel is the first diagnostic test to provide species-specific Candida detection and identification directly from whole blood in 3 to 5 hours, without the need for blood culture.
“We are greatly encouraged by the benefits these data show for the early detection of Candida with our T2Candida Panel,” said John McDonough, chief executive officer of T2 Biosystems. “The findings from this study demonstrate not only significant reduction in hospital costs, but most importantly, the potential to save so many patient lives by providing faster diagnostic results - supporting our goal of changing the paradigm in sepsis diagnosis. We look forward to working closely with the medical community to help implement this important change.”
UTMB develops new online tool for nurses

|
As tremendous advances are made in medicine, practitioners have new tools, but they also have more information to absorb and incorporate to provide evidence-based patient care: integrating best research evidence with clinical expertise and patient’s perspectives.
For the bedside nurse, this information can be lifesaving but time consuming. This has been a huge problem - until now.
The University of Texas Medical Branch has developed a new program that trains nurses how to pose questions that will point them to the needed information quickly. The Disciplined Clinical Inquiry - Evidence-Based Practice Literacy pathway is an online tool that helps nurses rapidly access filtered research evidence that present information in concise, easy to understand formats. An article describing this new program is available in the Journal for Nurses in Professional Development.
The EBP approach is becoming the “new normal” in patient care. UTMB’s online program offers a streamlined yet full education of the EBP skillset using online modules that take about three hours to learn. The standard DCI-EBP programs may take 50 hours to master.
Online health information - keep it simple!

|
Australian health websites are too difficult for many people to read.
This is the finding from a study published in Australian and New Zealand Journal of Public Health.
Matthew Dunn and Christina Cheng from Deakin University evaluated Australian online health information to see if it matched the reading level of Australians.
“Limited availability of ‘easy-to-read’ health materials suggests that many Australians may not be benefiting from the convenience of the internet,” Dr Dunn said.
Your privacy online: Health information at serious risk of abuse

|
There is a significant risk to your privacy whenever you visit a health-related web page. An analysis of over 80,000 such web pages shows that nine out of ten visits result in personal health information being leaked to third parties, including online advertisers and data brokers.
This puts users are risk for two significant reasons: first, people’s health interests may be publicly identified along with their names. This could happen because criminals get ahold of the information, it is accidentally leaked, or data brokers collect and sell the information. Second, many online marketers use algorithmic tools which automatically cluster people into groups with names like “target” and “waste”. Predictably, those in the “target” category are extended favorable discounts at retailers and advance notice of sales. Given that 62 percent of bankruptcies are the result of medical expenses, it is possible anyone visiting medical websites may be grouped into the “waste” category and denied favorable offers.
For individuals, this means profiles are built based on web page visits, potentially resulting in someone being labeled a commercial risk due to the fact that they have used a site like WebMD.com or CDC.gov to look up health information for themselves, a family member, or a friend. Given that data brokers are free to sell any information they collect regarding visits to health websites, those visiting such sites are potentially at risk of being discriminated against by potential employers, retailers, or anybody else with the money to buy the data.
Physician guidelines for Googling patients need revisions

|
With the Internet and social media becoming woven into the modern medical practice, Penn State College of Medicine researchers contend that professional medical societies must update or amend their Internet guidelines to address when it is ethical to “Google” a patient. “As time goes on, Googling patients is going to become more and more common, especially with doctors who grew up with the Internet,” says Maria J. Baker, associate professor of medicine. Baker has dealt with the question first hand in her role as a genetic counselor and medical geneticist. In a case that inspired her recent paper in the Journal of General Internal Medicine, a patient consulted her regarding prophylactic mastectomies. The patient’s family history of cancer could not be verified and then a pathology report revealed that a melanoma the patient listed had actually been a non-cancerous, shape-changing mole.
Turning to the Internet, Baker found evidence of the patient capitalizing on being a cancer victim for a cancer she did not have. The question, Baker says, is in what circumstances is it appropriate for a doctor to research a patient using online search engines? “Googling a patient can undermine the trust between a patient and his or her provider, but in some cases it might be ethically justified,” Baker says. “Healthcare providers need guidance on when they should do it and how they should deal with what they learn.”
With regard to future guidelines, Baker and her co-authors suggest 10 situations that may justify patient-targeted Googling:
Advance Directives Can Benefit Patients, Families, and Health Care System

|
Nearly one out of four older Americans say that either they or a family member have experienced excessive or unwanted medical treatment, according to the latest issue of The Gerontological Society of America’s Public Policy & Aging Report (PP&AR), which goes on to show that Americans strongly support holding doctors accountable when they fail to honor patients’ end-of-life health care wishes.
This PP&AR, titled “Advanced Illness Care: Issues and Options,” features 12 articles that present new ways of understanding the complexity of securing appropriate advanced illness care and the decision-making dilemmas it presents. It also provides a valuable benefit by reviewing specific programs, demonstrations, and tools that family members and providers can use in providing care to persons with advanced illness. These models are person- and family-centered, and preliminary evaluations find that they may be cost-effective as well. Support for the publication was provided by Compassion & Choices.
“It is important to ensure that patients and their wishes are what drive the health care system, particularly at the end of life,” said Daniel R. Wilson, the national and federal programs director for Compassion & Choices. “We were pleased to partner with The Gerontological Society of America to publish this issue of the PP&AR, which includes cutting edge writers and thinkers in the advanced illness and end-of-life field.”
Rare diseases: no reason for lower demands for studies

|
On behalf of the Federal Ministry of Health (BMG), the German Institute for Quality and Efficiency in Health Care (IQWiG) examined whether specific methodological aspects have to be considered in the conduct, analysis and assessment of the certainty of results of studies on rare diseases. Within the framework of the same commission, the Institute also analysed the underlying studies for the approval of so-called orphan drugs, i.e. drugs for rare diseases, in Europe.
The result: For a different approach than in more common diseases, there are neither scientific reasons nor specific designs and methods that would not also be relevant for more common diseases. This is the case for both drug and non-drug treatments. If compromises have to be made with regard to the reliability of the conclusions because of a particularly small number of participants, raising the significance level is preferable to a limitation of the external or even internal validity of the studies.
Focus on rare diseases
In the European Union diseases are classified as rare if they occur in not more than 5 per 10 000 inhabitants. Very rare diseases are diseases that affect fewer than 2 per 100 000 inhabitants. Of approximately 30 000 known diseases, 7000 to 8000 are considered rare, so that in Germany alone up to 4 million people are affected.
U.S. nutrition program for mothers, infants sees falling demand

|
A government nutrition program for pregnant mothers and small children has not kept pace with technology and U.S. poverty experts say its paper voucher system is driving low-income women away from the program when they need it most.
The Special Supplemental Nutrition Program for Women, Infants and Children, known as WIC, has seen a sharp drop in participation since 2010, unlike food stamps and other anti-poverty programs that ballooned during the 2007-9 recession and the economic recovery that followed, government figures show.
“WIC providers are tearing their hair, beating their chests, ‘what are they doing wrong?’” said Laurie True, California WIC Association director.
Poverty experts say the shrinking demand does not reflect less need. They are pushing for faster changes to an outdated, cumbersome distribution process they say stigmatizes recipients.





