Breast Cancer
Fat grafting technique improves results of breast augmentation

|
In women undergoing breast augmentation, a technique using transplantation of a small amount of the patient’s own fat cells can produce better cosmetic outcomes, reports a study in the April issue of Plastic and Reconstructive Surgery®, the official medical journal of the American Society of Plastic Surgeons (ASPS).
In particular, the fat grafting technique can achieve a more natural-appearing cleavage—avoiding the “separated breasts” appearance that can occur after breast augmentation, according to the report by Dr. Francisco G. Bravo of Clinica Gomez Bravo, Madrid.
Fat Grafting Adds to Cosmetic Results of Breast Augmentation
Dr Bravo analyzed the outcomes of breast augmentation surgery in 59 women. Thirty-eight women underwent conventional surgery using breast implants only. In the remaining 21 patients, Dr. Bravo used a combination technique using breast implants plus “selective para-sternal fat grafting.”
In this approach, a small amount of the patient’s own fat was harvested from elsewhere in the body - such as the thighs or abdomen. After processing, the fat cells were carefully placed along the inner (medial) borders of the breasts. The goal was to achieve a more natural shape, and particularly to soften the “medial transition zone” between the sternum (breastbone) and the implant edges.
UW research shows sensor technology may help improve accuracy of clinical breast exams

|
Sensor technology has the potential to significantly improve the teaching of proper technique for clinical breast exams (CBE), according to a new study by researchers at the University of Wisconsin School of Medicine and Public Health.
The results of the study were published in a correspondence today in the New England Journal of Medicine.
Carla Pugh, director of patient safety and education at the University of Wisconsin Hospital and Clinics and principal investigator of the study, says the use of sensors allows a level of critical analysis unavailable to clinicians until recently.
“Variations in palpable force used during a CBE cannot be reliably measured by human observation alone,” Pugh says. “Our findings revealed that 15 percent of the physicians we tested were using a technique that put them at significant risk of missing deep tissue lesions near the chest wall. This research underscores the potential for sensor technology to be used not only to improve clinical performance, but to also allow for objective evidence-based training, assessment and credentialing.”
Generic Breast Cancer Drugs Boost Adherence
|
|
The introduction of cheaper, generic aromatase inhibitors, used to prevent breast cancer recurrence, appears to have improved adherence, a researcher said here.
In an analysis of pharmacy claims data, adherence to hormone therapy varied depending on the copayment required, according to Dawn Hershman, MD, of Columbia University in New York City.
But the lower-priced generics had smaller copayments and adherence was greater than for brand name products, Hershman reported at the annual San Antonio Breast Cancer Symposium here.
The findings suggest that efforts should be directed toward reducing financial constraints on patients, as a matter of public health policy, Hershman argued.
New models of drug-resistant breast cancer point to better treatments

|
Human breast tumors transplanted into mice are excellent models of metastatic cancer and are providing insights into how to attack breast cancers that no longer respond to the drugs used to treat them, according to research from Washington University School of Medicine in St. Louis.
The transplanted tumors maintain the genetic errors that caused the original cancer, even though they are growing in mice. As such, mice carrying human tumors can help identify drivers of tumor growth and serve as excellent test subjects for investigating new drugs. The mice are particularly good models of estrogen receptor-positive tumors (so named because they are fueled by estrogen) that have become resistant to the drugs used to treat them.
Matthew J. Ellis, MD, PhD, said the research, presented Dec. 12 at the San Antonio Breast Cancer Symposium, is a step toward precision medicine, allowing scientists to study tumors from patients whose treatment regimens are well-documented.
The researchers, including scientists from The Genome Institute at Washington University School of Medicine, presented the research titled, “Patient-derived xenograft study reveals endocrine therapy resistance of ER+ breast cancer caused by distinct ESR1 gene aberrations.”
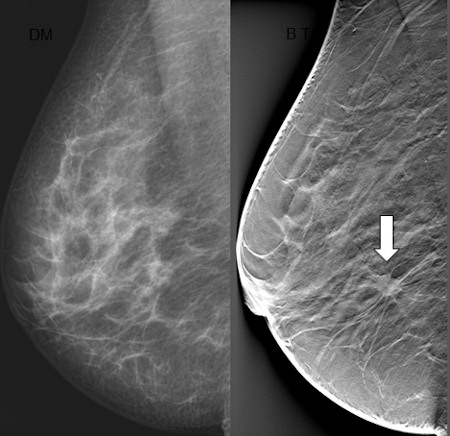
Breast tomosynthesis increases cancer detection and reduces recall rates
|
Researchers have found that digital breast tomosynthesis (DBT) led to reduced recall rates and an increase in cancer detection in a large breast cancer screening program. The results of this study were presented today at the annual meeting of the Radiological Society of North America (RSNA).
Digital mammography is the gold standard for breast cancer screening, but may yield suspicious findings that turn out not to be cancer. These false-positive findings are associated with a higher recall rate, or the rate at which women are called back for additional imaging or biopsy.
Digital breast tomosynthesis has shown promise at reducing recall rates in all groups of patients, including younger women and women with dense breast tissue. Tomosynthesis is similar to mammography in that it relies on ionizing radiation to generate images of the breast. However, unlike conventional mammography, tomosynthesis allows for three-dimensional (3-D) reconstruction of the breast tissue, which can then be viewed as sequential slices through the breast.
Because DBT technology is relatively new, it is typically used only as a supplemental screening tool, but since October 2011, every patient screened for breast cancer at Hospital of the University of Pennsylvania (HUP) in Philadelphia has been screened using DBT, according to Emily F. Conant, M.D., chief of breast imaging at HUP and the study’s lead author.
2 views are better than 1 in 3-D breast screening
|
|
One view 3D breast screening (tomosynthesis) means less radiation dose and about five seconds less compression, but a study from Yale University, New Haven, CT, found that obtaining both views is necessary to help ensure that a cancer won’t be missed.
There are practices in Europe that have reported performing only a single view, specifically the mediolateral oblique (MLO) view, said Dr. Noa Beck, the lead author of the study. Two views are standard in the U.S. for 3D breast screening; “we wanted to see if one view would be sufficient,” she said. Seven breast imagers reviewed 164 cancers visualized with tomosynthesis and noted on what views the cancers could be seen. The study found that 56% of cancers were equally well seen on both the MLO view and the craniocaudal (CC) view; 34% of the cancers were either better or only seen on the CC view, said Dr. Beck. “The CC view achieves better compression, and this likely explains the reason the CC view showed lesions more clearly. In a few cases, lesions were only seen on the MLO view because of where the cancers were located in the breast,” she said.
The study results emphasize that “obtaining both views is necessary to ensure that a cancer will be optimally visualized,” said Dr. Beck.
Study reveals genomic similarities between breast cancer and ovarian cancers
|
|
One subtype of breast cancer shares many genetic features with high-grade serous ovarian cancer, a cancer that is very difficult to treat, according to researchers supported by the National Institutes of Health. The findings suggest that the two cancers are of similar molecular origin, which may facilitate the comparison of therapeutic data for subtypes of breast and ovarian cancers.
The researchers, using data generated as part of The Cancer Genome Atlas (TCGA), described new insights into the four standard molecular subtypes based on a comprehensive characterization of samples from 825 breast cancer patients.
The study, a collaborative effort funded by the National Cancer Institute (NCI) and the National Human Genome Research Institute (NHGRI), both part of NIH, was published online Sept. 23, 2012, and in print Oct. 4, 2012, in the journal Nature.
“TCGA’s comprehensive characterization of their high-quality samples allows researchers an unprecedented look at these breast cancer subgroups,” said NIH Director Francis S. Collins, M.D., Ph.D.
Moderate exercise tied to lower breast cancer risk
|
|
Women who exercise moderately may be less likely than their inactive peers to develop breast cancer after menopause, a study published Monday suggests.
Researchers found that of more than 3,000 women with and without breast cancer, those who’d exercised during their childbearing years were less likely to develop the cancer after menopause.
The same was true when women took up exercise after menopause.
And it did not take a vigorous workout; regular exercise at any intensity level was linked to a lower breast cancer risk, the researchers say.
Risk for some cancers rises with U.S. obesity rate
|
|
The total number of Americans dying from or diagnosed with cancer is falling, but certain cancers linked to obesity and inactivity are on the rise, according to an annual report on the status of cancer in the United States.
U.S. cancer rates fell 0.6 percent per year between 2004 and 2008, according to the report, based on data from the National Cancer Institute, the Centers for Disease Control and Prevention and other sources.
For men, the incidence of prostate cancer dropped by an average 2.1 percent per year, while lung cancer rates fell 2 percent. In women, lung cancer rates declined by 1.2 percent a year, while the incidence of breast cancer, which is associated with obesity, was flat.
“Breast cancer incidence did drop when hormones were stopped, but it has now plateaued,” said Dr. Powel Brown, chairman of clinical cancer prevention in the department of breast medical oncology at the University of Texas MD Anderson Cancer Center in Houston.
New genomic test spares patients chemotherapy with no adverse effect on survival
|
|
Testing a breast cancer tumour for its genomic signature can help identify which patients will need adjuvant systemic therapy (additional chemotherapy) after surgery, and spare its use in those for whom it is not necessary, according to the results of a study to be presented to the 8th European Breast Cancer Conference (EBCC-8) today (Thursday). Dr. Sabine Linn, an Associate Professor of Medical Oncology at The Netherlands Cancer Institute, Amsterdam, The Netherlands, will say that this is the first study where such a test has been incorporated in decision-making about adjuvant systemic therapy, and that the results are promising.
Adjuvant chemotherapy is used in order to destroy any microscopic cancer cells that might still be present in the body after surgery. Although it is effective, the side effects can be distressing. “Based on our data, the use of the genomic test could lead to a reduction of nearly 30% in the use of adjuvant chemotherapy without compromising patient outcomes,” Dr. Linn will say. “This percentage may vary somewhat due to different guidelines used in different countries. These findings are important both for quality of life and for cutting down unnecessary healthcare costs.”
The researchers studied follow-up data from 427 patients with early breast cancer who had taken part in a study called RASTER (MicroarRAy prognoSTics in breast cancER). Their cancers had not yet spread to the lymph nodes (node-negative). By looking for a particular selection of 70 genes in a tumour, the Mammaprint® test can predict which patients are at low and which at high risk of distant disease (metastasis); this enables doctors to select which patients could be spared the side effects of chemotherapy without adversely affecting their chances of disease-free survival. The study aimed to assess the feasibility of implementing the test in daily clinical practice in The Netherlands, as well as its effect on adjuvant systemic treatment decisions.
Breast Cancer In Black Women Is A Different Disease
|
|
Black women have a higher risk of developing a certain type of breast cancer, one that is more aggressive and less amenable to targeted therapies such as anti-estrogen drugs (tamoxifen, aromatase inhibitors) and monoclonal antibodies like Herceptin. While the cause of this unfortunate epidemiologic disparity remains unclear, researchers have identified two risk factors that ought to be of interest to black women and the public health officials who help oversee their care.
First, some background information:
For white women, having several children at a young age protects against breast cancer, particularly if the pregnancies are completed before the age of twenty. Also, for white women, breast-feeding lowers the risk for breast cancer, but only very slightly.
Combination of Everolimus and Exemestane Improves Progression-Free Survival for Women with Metastatic Breast Cancer
|
|
San Antonio, TX - In an international Phase III randomized study, everolimus, when combined with the hormonal therapy exemestane, has been shown to dramatically improve progression-free survival, according to research from The University of Texas MD Anderson Cancer Center.
The study, known as Breast Cancer Trials of Oral Everolimus (BOLERO-2), was presented today at the 2011 CTRC-AACR San Antonio Breast Cancer Symposium by Gabriel Hortobagyi, M.D., professor and chair of MD Anderson’s Department of Breast Medical Oncology. Earlier findings were simultaneously reported in the New England Journal of Medicine.
Everolimus, an immunosuppressant agent first used to prevent rejection of organ transplants, also has anti-angiogenic properties. It inhibits the mammalian target of rapamycin (mTOR) protein, a central regulator of tumor cell division and blood vessel growth in cancer cells; the mTOR pathway is activated in hormone-resistant breast cancer, explained Hortobagyi. Currently, the oral agent is approved for both the treatment of kidney cancer and pancreatic neuro-endocrine tumors, with MD Anderson’s research leading the way for the latter’s usage approval by the FDA.
Breast Cancer and the Environment: IOM report release Dec. 7
|
|
Although women have little or no control over some of the risk factors for breast cancer, such as those related to aging and genetics, they may be able to reduce their chances for developing the disease by avoiding certain environmental risks. BREAST CANCER AND THE ENVIRONMENT: A LIFE COURSE APPROACH, a new report from the Institute of Medicine, assesses the breast cancer risk posed by various environmental factors, identifies actions that offer potential to reduce women’s risk for the disease, and recommends targets for future research. The report, sponsored by Susan G. Komen for the Cure, will be released with a press briefing and presented at a plenary session at the 2011 San Antonio Breast Cancer Symposium (SABCS).
###
DETAILS:
The report will be released on Wednesday, Dec. 7, at a one-hour press briefing starting at 1:30 p.m. EST/12:30 p.m. CST in Room 217D of the Henry B. Gonzalez Convention Center, 200 E. Market St., San Antonio. Reporters who cannot attend may participate through a live teleconference by dialing 888-647-7462 (U.S. and Canada) or 1-201-604-0169 (international). Participants from the committee that wrote the report are:
Irva Hertz-Picciotto (chair), professor and chief, division of environmental and occupational health, University of California, Davis
Many advanced breast cancer patients do not receive recommended treatment
|
|
Radiation after a mastectomy for women with advanced breast cancer saves lives, but almost half of these patients do not receive it. That is the conclusion of a new study published early online in CANCER, a peer-reviewed journal of the American Cancer Society. The study’s results indicate that treatments that have proven their life-saving potential in clinical trials may not be available to many patients.
After clinical trials in the 1990s revealed the benefits of radiation after mastectomy in advanced breast cancer patients, several major treatment guidelines were published that recommended radiation for these women after their surgery. To investigate whether these recommendations are being followed, Shervin Shirvani, MD, and Benjamin Smith, MD, of the MD Anderson Cancer Center in Houston, led a team that analyzed information from 38,322 women aged ≥ 66 years treated with mastectomy for invasive breast cancer between 1992 and 2005. (The researchers obtained data from the Surveillance, Epidemiology, and End Results [SEER]-Medicare database, which links cancer registry data to a master file of Medicare enrollment.)
While radiation use increased from 36.5 percent to 57.7 percent between 1996 and 1998 with the publication of landmark clinical trials, no further increase in use was observed between 1999 and 2005 despite the publication of multiple guidelines endorsing it.
Social isolation, stress-induced obesity increases breast cancer risk in mice
|
|
Stress from social isolation, combined with a high-fat diet, increases levels of a brain neurotransmitter – neuropeptide Y, or NPY – in mice that then promotes obesity, insulin resistance, and breast cancer risk, say researchers at Georgetown Lombardi Comprehensive Cancer Center, a part of Georgetown University Medical Center (GUMC).
Major increases in NPY levels are seen when isolation and the high fat diet are combined. Still, the mice that were isolated for two weeks and fed a control diet had elevated NPY levels and increased terminal end buds, a structure in the mammary gland where mammary cancers form.
The researchers say their findings, reported at the American Association for Cancer Research (AACR) 102nd Annual Meeting 2011, appear to link a number of findings in humans, such as the fact that social isolation is associated with an increased risk of cancer development and mortality, and that obesity is a risk factor for breast cancer.”





