Cancer
New biomarkers may influence drug design and alternative treatments of cancer, study shows

|
Researchers have discovered gene-targets (biomarkers) that may enable alternative treatments or the potential design of new drugs that target metastasis-promoting tumor genes.
This is the key finding in a study led by researchers from Georgia State University in collaboration with the University of Oklahoma College of Medicine and published in journal Oncotarget.
The spread of cancer cells from the initial site of occurrence (primary site) to other secondary tissues is called metastasis, and contributes to poor or limited response of cancer cells to treatments, which results in death. For example, cancer cells initially in the lungs can begin to spread to other organs, including the brain and liver.
Metabolic profiles distinguish early stage ovarian cancer with unprecedented accuracy

|
Studying blood serum compounds of different molecular weights has led scientists to a set of biomarkers that may enable development of a highly accurate screening test for early-stage ovarian cancer.
Using advanced liquid chromatography and mass spectrometry techniques coupled with machine learning computer algorithms, researchers have identified 16 metabolite compounds that provided unprecedented accuracy in distinguishing 46 women with early-stage ovarian cancer from a control group of 49 women who did not have the disease. Blood samples for the study were collected from a broad geographic area - Canada, Philadelphia and Atlanta.
While the set of biomarkers reported in this study are the most accurate reported thus far for early-stage ovarian cancer, more extensive testing across a larger population will be needed to determine if the high diagnostic accuracy will be maintained across a larger group of women representing a diversity of ethnic and racial groups.
Moffitt researchers develop first genetic test to predict tumor sensitivity to radiation therapy

|
Recent advances in the understanding of cancer have led to more personalized therapies, such as drugs that target particular proteins and tests that analyze gene expression patterns in tumors to predict a patient’s response to therapy. Moffitt Cancer Center researchers have contributed to these advances by developing the first test that analyzes the sensitivity of tumors to radiation therapy. They discovered that colon cancer metastases have varying sensitivity to radiation therapy based on their anatomic location.
Researchers from Moffitt previously developed a radiation sensitivity index (RSI) that predicts how sensitive tumors are to radiation based on expression patterns of different genes. In a paper published July 15 in The International Journal of Radiation Oncology, Biology and Physics, they used the RSI to determine the radiation sensitivity of 704 metastatic and 1362 primary colon tumors.
They discovered that metastatic colon tumors are more resistant to radiation than primary colon tumors. The researchers also report that radiation sensitivity may be dependent on the anatomic location of the tumor metastasis. This is one of the first research studies to highlight the importance of the location of the metastasis as well as the location of the original primary tumor, in predicting response to radiation therapy. The researchers confirmed some of these findings by analyzing how effective radiation therapy was in 29 colon cancer tumors that metastasized to either the liver or lung. Their findings validated that those patients who had metastatic disease in their lungs had a better response to radiation then patients who had metastatic disease in their liver, as predicted by RSI.
New drug for neuroblastoma shows promise in phase I study

|
Researchers at Spectrum Health Helen DeVos Children’s Hospital have completed the first clinical trial of a new treatment for children suffering from neuroblastoma. In a clinical trial led by Giselle Sholler, MD, pediatric oncologist at Helen DeVos Children’s Hospital and the Neuroblastoma and Medulloblastoma Translational Research Consortium (NMTRC), DFMO, an investigational agent, showed minimal side effects with long-term survival of three patients. This is the first clinical study of an oral dosing form of DFMO in any pediatric population.
“This DFMO trial is an important advancement in neuroblastoma research,” explained Dr. Sholler. “We believe that by using DFMO to target an important cancer stem cell pathway to ‘turn cells off,’ we may prevent children from relapsing. Cancer cells have pathways that drive the cancer to grow and DFMO targets a specific pathway to turn these cells off.”
Dr. Sholler recently published her laboratory studies describing how this drug works in neuroblastoma in preventing tumor formation in lab models and also published the full results of the phase one trial.
Experimental treatment sends deadly leukemia into remission
|
An experimental new treatment approach for a rare, deadly leukemia can send the disease into remission even in patients for whom the standard therapy has failed, buying them more time to have the stem cell transplant that could save their lives, a small pilot study has found.
“It was unbelievable, really, seeing a patient who had already failed Campath [the drug typically used to treat the disease] literally going back into remission,” said Thomas P. Loughran Jr., M.D., director of the University of Virginia Cancer Center and one of the leaders of the study. “We were able to get every single patient back into remission.”
The new approach to battling T-cell prolymphocytic leukemia combines immunotherapy - boosting the body’s immune system - with epigenetics, the manipulation of gene activity. It’s a cutting-edge combination that holds great promise not just for treating T-cell prolymphocytic leukemia but, possibly, many other cancers as well. “There’s been a revolution in the last few years seeing success with immunotherapy, and people speculated that perhaps if you combined epigenetic and immunotherapy, that might be even more spectacular,” Loughran said. “This is proof of principle that this might be true.”
Study could reduce unnecessary cancer screening

|
A large clinical trial led by researchers at The Ottawa Hospital and the University of Ottawa has found that contrary to expectations, a CT scan of the abdomen and pelvis does not improve cancer detection in people with unexplained blood clots in their legs and lungs. The results, published in the June 22 edition of the New England Journal of Medicine, are expected to improve patient care and reduce screening costs around the world.
More than 500,000 Canadians and Americans are diagnosed with blood clots in the lungs and legs each year (called venous thromboembolism). In some cases, the clots are caused by trauma, surgery prolonged immobility or a known cancer, but in about half of cases, the cause of the blood clots is unknown.
‘Unexplained blood clots have long been thought of as a possible early warning sign of cancer, with previous studies suggesting that up to 10 percent of patients with unexplained clots will be diagnosed with cancer within the year,’ explained Dr. Marc Carrier, lead author of the study and a hematologist and senior scientist at The Ottawa Hospital. ‘Some clinical guidelines recommend a CT scan of the abdomen and pelvis in these patients, in addition to other cancer screening, but there has been very little evidence to know if the added CT scan is helpful. We did this study to find out.’
UA researchers discover component of cinnamon prevents colorectal cancer in mice

|
Research conducted at the University of Arizona College of Pharmacy and the UA Cancer Center indicates that a compound derived from cinnamon is a potent inhibitor of colorectal cancer.
Georg Wondrak, Ph.D., associate professor, and Donna Zhang, Ph.D., professor, both of the UA College of Pharmacy Department of Pharmacology and Toxicology, recently completed a study in which they proved that adding cinnamaldehyde, the compound that gives cinnamon its distinctive flavor and smell, to the diet of mice protected the mice against colorectal cancer. In response to cinnamaldehyde, the animals’ cells had acquired the ability to protect themselves against exposure to a carcinogen through detoxification and repair.
‘This is a significant finding,’ says Zhang, who, along with Wondrak, is a member of the UA Cancer Center. ‘Because colorectal cancer is aggressive and associated with poor prognoses, there is an urgent need to develop more effective strategies against this disease.’
Profiling approach to enable right lung cancer treatment match

|
Manchester researchers have tested a new way to genetically profile lung cancer samples, potentially allowing doctors to more easily identify the most appropriate treatment for patients.
Non-small cell lung cancer (NSCLC) represents over 85% of lung cancer cases. The recent introduction of targeted therapies has led to improved patient survival, but only patients whose tumours have a specific genetic change are eligible for such treatments.
Identifying individual patients who may benefit from targeted therapy is becoming an essential part of treatment planning, but many current genetic analysis methods such as next generation sequencing require relatively large amounts of tumour material.
Dr Fiona Blackhall, a senior lecturer in The University of Manchester’s Institute of Cancer Sciences and a consultant based at The Christie NHS Foundation Trust - both part of the Manchester Cancer Research Centre - said: “Unfortunately the biopsy samples we take from these patients are generally quite small. In this study we looked at an alternative genetic screen that utilises a much smaller tissue biopsy to see if it can detect a range of changes in 26 key genes.”
Fat grafting technique improves results of breast augmentation

|
In women undergoing breast augmentation, a technique using transplantation of a small amount of the patient’s own fat cells can produce better cosmetic outcomes, reports a study in the April issue of Plastic and Reconstructive Surgery®, the official medical journal of the American Society of Plastic Surgeons (ASPS).
In particular, the fat grafting technique can achieve a more natural-appearing cleavage—avoiding the “separated breasts” appearance that can occur after breast augmentation, according to the report by Dr. Francisco G. Bravo of Clinica Gomez Bravo, Madrid.
Fat Grafting Adds to Cosmetic Results of Breast Augmentation
Dr Bravo analyzed the outcomes of breast augmentation surgery in 59 women. Thirty-eight women underwent conventional surgery using breast implants only. In the remaining 21 patients, Dr. Bravo used a combination technique using breast implants plus “selective para-sternal fat grafting.”
In this approach, a small amount of the patient’s own fat was harvested from elsewhere in the body - such as the thighs or abdomen. After processing, the fat cells were carefully placed along the inner (medial) borders of the breasts. The goal was to achieve a more natural shape, and particularly to soften the “medial transition zone” between the sternum (breastbone) and the implant edges.
Germline TP53 mutations in patients with early-onset colorectal cancer

|
In a group of patients diagnosed with colorectal cancer at 40 or younger, 1.3 percent of the patients carried germline TP53 gene mutations, although none of the patients met the clinical criteria for an inherited cancer syndrome associated with higher lifetime risks of multiple cancers, according to a study published online by JAMA Oncology.
Li-Fraumeni syndrome is an inherited cancer syndrome usually characterized by germline TP53 mutations in which patients can develop early-onset cancers and have an increased risk for a wide array of other cancers including colorectal. The gene’s contribution to hereditary and early-onset colorectal cancer is needed for clinicians to counsel patients undergoing TP53 testing as part of a multigene risk assessment, according to the study background.
Sapna Syngal, M.D., M.P.H., of the Dana-Farber Cancer Institute, Boston, and coauthors estimated the proportion of patients with early-onset colorectal cancer who carry germline TP53 mutations. Participants were recruited from the Colon Cancer Family Registry from 1998 through 2007 and were those individuals who were diagnosed with colorectal cancer at 40 or younger and lacked a known hereditary cancer syndrome.
Among 457 eligible patients, six (1.3 percent) of them carried germline missense TP53 alterations and none of the patients met the clinical criteria for Li-Fraumeni syndrome, according to the results.
Clinical trial suggests combination therapy is best for low-grade brain tumors

|
New clinical-trial findings provide further evidence that combining chemotherapy with radiation therapy is the best treatment for people with a low-grade form of brain cancer. The findings come from a phase II study co-led by a researcher at Ohio State University Comprehensive Cancer Center - Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (OSUCCC - James) and researchers at the University of Maryland and at London Regional Cancer Program in Ontario, Canada.
The study shows that patients with low-grade gliomas and at high risk for tumor recurrence have an overall survival of 73 percent after three years when treated with radiation plus temozolomide, a chemotherapy drug. This is compared with a three-year survival of 54 percent for historical controls treated with radiation alone.
The findings are published in the International Journal of Radiation Oncology, Biology, Physics.
UW research shows sensor technology may help improve accuracy of clinical breast exams

|
Sensor technology has the potential to significantly improve the teaching of proper technique for clinical breast exams (CBE), according to a new study by researchers at the University of Wisconsin School of Medicine and Public Health.
The results of the study were published in a correspondence today in the New England Journal of Medicine.
Carla Pugh, director of patient safety and education at the University of Wisconsin Hospital and Clinics and principal investigator of the study, says the use of sensors allows a level of critical analysis unavailable to clinicians until recently.
“Variations in palpable force used during a CBE cannot be reliably measured by human observation alone,” Pugh says. “Our findings revealed that 15 percent of the physicians we tested were using a technique that put them at significant risk of missing deep tissue lesions near the chest wall. This research underscores the potential for sensor technology to be used not only to improve clinical performance, but to also allow for objective evidence-based training, assessment and credentialing.”
HPV vaccination not associated with increase in sexually transmitted infections

|
A barrier to human papillomavirus (HPV) vaccination has been the concern that it may promote unsafe sexual activity, but a new study of adolescent girls finds that HPV vaccination was not associated with increases in sexually transmitted infections (STIs), according to an article published online by JAMA Internal Medicine.
Nearly one-quarter of U.S. females between the ages 14 and 19 and 45 percent of women between the ages of 20 and 24 are affected by HPV. The HPV vaccination can prevent cervical, vulvar and vaginal cancers and genital warts caused by certain HPV strains. Still, HPV vaccination rates remain low in the United States and, by 2013, only 57 percent of females between the ages of 13 and 17 had received at least one dose, whereas only 38 percent had received all three recommended doses, according to the study background.
Anupam B. Jena, M.D., Ph.D., of Harvard Medical School, Boston, and coauthors used a large insurance database of females (ages 12 to 18) from 2005 through 2010 to examine STIs among girls who were vaccinated and those who were not.
Study identifies 8 signs associated with impending death in cancer patients

|
Researchers at The University of Texas MD Anderson Cancer Center have identified eight highly specific physical and cognitive signs associated with imminent death in cancer patients. The findings, published in the journal Cancer, could offer clinicians the ability to better communicate with patients and families. They may also guide both the medical team and caregivers on complex decision making, such as discontinuation of tests and therapy, plans for hospital discharge and hospice referral.
Previous studies in end-of-life care have focused on physicians prognosticating better. However, according to David Hui, M.D., assistant professor, Palliative Care and Rehabilitation Medicine, research on how to tell if a patient has entered the final days of life has been minimal. Knowing with a high degree of confidence that death is imminent could have significant implications for clinical practice. It may also help families and caregivers make more informed decisions.
“In the past, studies trying to understand the signs associated with impending death were conducted in people who were recognized as dying, so there’s a potential bias built into this model. With our study, we observed a list of signs in patients from the time they were admitted to the palliative care unit. They were observed systematically, twice a day, without knowing if the patient would die or be discharged,” says Hui, the study’s corresponding author.
Researchers identify efficient methylating enzyme for cancer development
|
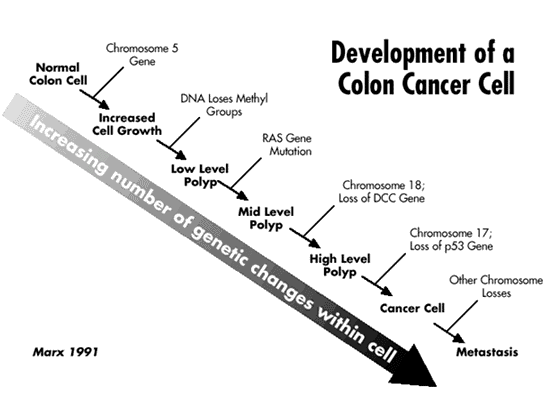
A recent study may help begin to explain how cancer develops though the abnormal turning on and off of genes. Researchers have discovered that the increase of methyl tags in cancer cells is due to highly efficient DNA methyl transferase 1 (DNMT1) enzymes found in these cells. The findings appear in the Journal of Proteomics and Bioinformatics.
Both plants and animals have genetic machinery that modifies the information and function of their genomes without actually changing their genetic code. This modification process is known as “epigenetics.” One of the best studied of these epigenetic processes involves the chemical tagging of DNA nucleotides across the genome using methyl groups. These “methyl tags” are attached to cytosine nucleotides in specific patterns around genes and other expressed sequences by a specialized group of enzymes called methyltransferases.
Genes that are expressed and turned into proteins are free of “methyl” tags, but when such methyl tags attach to DNA, gene expression is turned off. “Whether methyl tags are added to genes varies during normal development and during the development of diseases like cancer, and understanding these processes is currently a major topic of research,” explained corresponding author Sibaji Sarkar, PhD, instructor of medicine at Boston University School of Medicine (BUSM). According to Sarkar it was previously discovered that cancer cells have more methyl tags than normal cells and level of the enzyme which adds the tag, DNA methyl transferase1 (DNMT1) is also higher, but no one knew that both increases are not proportional.





