Immunology
Drug prevents passage of HBV during pregnancy
|
|
The antiviral drug telbivudine prevents perinatal transmission of hepatitis B virus (HBV), according to a study1 in the June issue of Clinical Gastroenterology and Hepatology, the official clinical practice journal of the American Gastroenterological Association.
“If we are to decrease the global burden of hepatitis B, we need to start by addressing mother-to-infant transmission, which is the primary pathway of HBV infection,” said study author Yuming Wang from Institute for Infectious Diseases, Southwest Hospital, Chongqing, China. “We found that telbivudine not only eliminated vertical transmission of HBV from pregnant women to theirs infants, but that it is also safe and well tolerated by women and infants.”
Researchers performed a prospective study of 450 HBV-positive pregnant women with high viral load, or significant HBV in the blood, during the second or third trimester of pregnancy. Two hundred and seventy nine women received telbivudine (600 mg daily) during weeks 24 through 32 of gestation, and 171 women who were unwilling to take antiviral drugs participated as controls. At six months after birth, none of the infants whose mothers were given telbivudine tested positive for HBV, compared to 14.7 percent of infants in the control group.
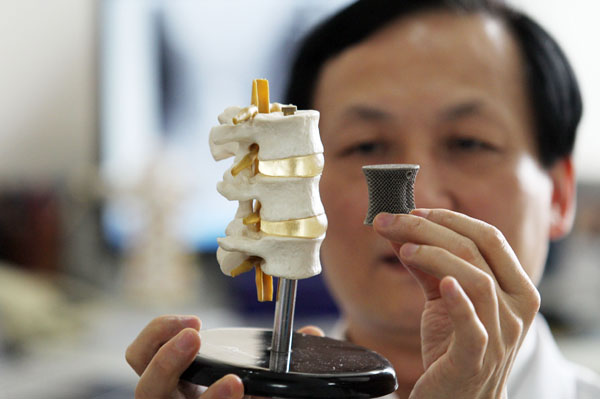
Designing better medical implants
|
Biomedical devices that can be implanted in the body for drug delivery, tissue engineering, or sensing can help improve treatment for many diseases. However, such devices are often susceptible to attack by the immune system, which can render them useless.
A team of MIT researchers has come up with a way to reduce that immune-system rejection. In a study appearing in the May 18 issue of Nature Materials, they found that the geometry of implantable devices has a significant impact on how well the body will tolerate them.
Although the researchers expected that smaller devices might be better able to evade the immune system, they discovered that larger spherical devices are actually better able to maintain their function and avoid scar-tissue buildup.
“We were surprised by how much the size and shape of an implant can affect its triggering of an immune response. What it’s made of is still an important piece of the puzzle, but it turns out if you really want to have the least amount of scar tissue you need to pick the right size and shape,” says Daniel Anderson, the Samuel A. Goldblith Associate Professor in MIT’s Department of Chemical Engineering, a member of MIT’s Koch Institute for Integrative Cancer Research and Institute for Medical Engineering and Science (IMES), and the paper’s senior author.
Baclofen shows promise in patients with alcohol-induced liver disease

|
Results revealed today at The International Liver Congress™ 2015, show that in patients with alcohol-induced liver disease (ALD), Baclofen has a positive impact on alcohol consumption and overall measures of liver function and harm.
ALD is a major cause of alcohol-related mortality and helping patients with ALD to stop drinking is a primary goal of treatment. The primary aim of this study was to measure the effectiveness and tolerability of Baclofen in maintaining abstinence in this difficult to treat group, and to determine if this resulted in a reduction in standard measures of liver damage.
The results show promising outcomes for these patients, helping them to reduce their alcohol consumption as well as improving overall indicators of liver function and lowering physical dependence. A randomised controlled trial is now needed to confirm the benefit of Baclofen in this patient group.
###
About The International Liver Congress
This annual congress is the biggest event in the EASL calendar, attracting scientific and medical experts from around the world to learn about the latest in liver research.
Scientists discover potential new target for cancer immunotherapy

|
Scientists have found a way to target elusive cells that suppress immune response, depleting them with peptides that spare other important cells and shrink tumors in preclinical experiments, according to a paper published online by Nature Medicine.
“We’ve known about these cells blocking immune response for a decade, but haven’t been able to shut them down for lack of an identified target,” said the paper’s senior author, Larry Kwak, M.D., Ph.D., chair of Lymphoma/Myeloma and director of the Center for Cancer Immunology Research at The University of Texas MD Anderson Cancer Center.
The cells, called myeloid-derived suppressor cells (MDSCs), are found abundantly in the microenvironment around tumors. Created with other blood cells in the bone marrow, they interfere with activation and proliferation of T cells, the immune system’s attack cells. MDSCs have been shown in mouse models to accelerate cancer progression and metastasis.
“This is the first demonstration of a molecule on these cells that allows us to make an antibody, in this case a peptide, to bind to them and get rid of them,” Kwak said. “It’s a brand new immunotherapy target.”
Immune system ‘overdrive’ in pregnant women puts male child at risk for brain disorders

|
Johns Hopkins researchers report that fetal mice - especially males - show signs of brain damage that lasts into their adulthood when they are exposed in the womb to a maternal immune system kicked into high gear by a serious infection or other malady. The findings suggest that some neurologic diseases in humans could be similarly rooted in prenatal exposure to inflammatory immune responses.
In a report on the research published online last week in the journal Brain, Behavior and Immunity, the investigators say that the part of the brain responsible for memory and spatial navigation (the hippocampus) was smaller over the long term in the male offspring exposed to the overactive immune system in the womb. The males also had fewer nerve cells in their brains and their brains contained a type of immune cell that shouldn’t be present there.
“Our research suggests that in mice, males may be more vulnerable to the effects of maternal inflammation than females, and the impact may be life long,” says study leader Irina Burd, M.D., Ph.D., an assistant professor of gynecology/obstetrics and neurology at the Johns Hopkins University School of Medicine and director of the Integrated Research Center for Fetal Medicine. “Now we wonder if this could explain why more males have diseases such as autism and schizophrenia, which appear to have neurobiological causes.”
For the study, researchers sought to mimic the effects of a maternal infection or other condition that causes inflammation in a pregnant mother. This type of inflammation between 18 and 32 weeks of gestation in humans has been linked to preterm birth as well as an imbalance of immune cells in the brain of the offspring and even death of nerve cells in the brains of those children. Burd and her colleagues used a mouse model to study what happens to the brains of those offspring as they age into adulthood to see if the effects persisted.
Testosterone-regulated genes may affect vaccine-induced immunity

|
A new study has identified a link between certain genes affected by testosterone and antibody responses to an influenza vaccine. The findings, published in Proceedings of the National Academy of Sciences, suggest that testosterone levels may partially explain why men often have weaker responses to vaccines than women. The study, led by researchers at Stanford University, was supported in part by the National Institute of Allergy and Infectious Diseases (NIAID), a component of the National Institutes of Health.
Previous research has shown that men typically experience more severe viral and other microbial infections than women, who tend to mount stronger immune responses to infections and vaccinations. In the new study, researchers analyzed the antibody responses of 53 women and 34 men of various ages to the 2008-2009 seasonal influenza vaccine. Compared to the men, the women produced antibodies that in laboratory tests could more effectively neutralize the influenza virus.
To explain this difference, the scientists searched for patterns in gene expression, or the degree to which specific genes are turned on or off. They found that men with weak vaccine responses tended to have high expression levels of a certain cluster of genes involved in the metabolism of lipids (fats). Previous studies have suggested that testosterone may regulate the expression of many of these genes. The researchers found that men with high levels of testosterone and elevated expression of the gene cluster had weaker antibody responses to the vaccine than women and men with low testosterone. These results suggest that testosterone may suppress immune responses to vaccines by altering expression patterns of specific genes, but further research is needed to determine the mechanism.
###
Fungus-fighting drug may make mild flu meaner

|
Mice given a drug commonly used in patients to fight systemic fungal infections more often succumb to what would otherwise be a mild case of the flu. The evidence reported in the Cell Press journal Cell Reports on November 21st shows that the drug called Amphotericin B, which has an estimated $330 million in sales around the world each year, can render a protein important for antiviral defense ineffective in both cells and mice.
The findings suggest that patients receiving the antifungal therapy may be functionally immunocompromised and more vulnerable to influenza and other viral infections, the researchers said.
“Many critically ill cancer and bone marrow transplant patients are treated with Amphotericin B-based therapies each year,” said Abraham Brass of the University of Massachusetts Medical School (UMMS). “Given these results in cells and mice, it may be worthwhile to consider that patients receiving, or who may receive, Amphotericin B-based therapies be appropriately vaccinated against influenza virus. Also, clinical consideration may be given to close monitoring of patients receiving Amphotericin B-based therapies for any symptoms suggestive of flu so that they might be considered for the early administration of an antiflu therapy.”
The researchers showed that Amphotericin-B prevents the antiviral protein in cells known as IFITM3 from fending off influenza A virus.
Stanford scientists think mysterious virus could be a signal of a weak immune system

|
More than 260,000 Americans are alive today thanks to transplant operations that have replaced their failing kidneys, hearts, lungs or livers with healthy organs donated by volunteers or accident victims.
But treatment doesn’t end with surgery. Transplant recipients follow strict drug regimens designed to suppress their immune systems just enough to prevent rejection of the donated organ, but not so much as to leave them prone to infection.
Until now, maintaining this delicate balance has been something of a medical guessing game. But in a study to be published Nov. 21 in Cell, Stanford University scientists report the discovery of what may be a barometer of immune system strength: a little-known virus that proliferates as the medications suppress the immune system.
The work was led by senior author Stephen Quake, PhD, the Lee Otterson Professor in the School of Engineering and professor of bioengineering and of applied physics.
Nearly half of U.S. children late receiving vaccines
|
|
Nearly half of babies and toddlers in the United States aren’t getting recommended vaccines on time, according to a study - and if enough skip vaccines, whole schools or communities could be vulnerable to diseases such as whooping cough and measles.
“What we’re worried about is if (undervaccination) becomes more and more common, is it possible this places children at an increased risk of vaccine-preventable diseases?” said study leader Jason Glanz, with Kaiser Permanente Colorado in Denver.
“It’s possible that some of these diseases that we worked so hard to eliminate (could) come back.”
Glanz and his colleagues analyzed data from eight managed care organizations, including immunization records for about 323,000 children.
Steroid hormone receptor prefers working alone to shut off immune system genes
|
|
Researchers at Emory University School of Medicine have obtained a detailed molecular picture that shows how glucocorticoid hormones shut off key immune system genes.
The finding could help guide drug discovery efforts aimed at finding new anti-inflammatory drugs with fewer side effects.
The results are scheduled for publication Sunday, Dec. 9 by the journal Nature Structural & Molecular Biology.
Synthetic glucocorticoid hormones - for example, prednisone and dexamethasone - are widely used to treat conditions such as allergies, asthma, autoimmune diseases and cancer. They mimic the action of the natural hormone cortisol, which is involved in the response to stress and in regulating metabolism and the immune system. For this reason, synthetic glucocorticoids have a variety of severe side effects such as increased blood sugar and reduced bone density.
Study shows school-based health centers boost vaccination rates
|
|
New research from the University of Colorado School of Medicine shows that school-based health centers are highly effective in delivering comprehensive care, especially vaccines to adolescents.
The study, published today in the journal Pediatrics, highlights the value of a ‘captive audience’ in a school setting where students can be easily reminded to get recommended vaccinations.
“School-based health centers can provide comprehensive care to children and adolescents who are hard to reach,” said CU School of Medicine professor of pediatrics Allison Kempe, MD, MPH, and lead author of the study. “I think it’s a very important model especially in underserved and low income areas. School-based health centers are not prevalent across the United States but I think they should be.”
Kempe, director of the Children’s Outcomes Research Program at Children’s Hospital Colorado, said the scope of immunizations for adolescents has expanded markedly over the last few years, prompting discussions about a platform of inoculations for this population similar to those given to infants.
China vaccinates 4.5 million people in fight against polio
|
|
China vaccinated 4.5 million children and young adults over the last five weeks in the western region of Xinjiang in a fight against polio after the disease paralyzed 17 people and killed one of them, the World Health Organization said.
Polio has broken out in China for the first time since 1999 and scientists say the strain originated from Pakistan. The outbreak marked the latest setback to a global campaign to eradicate polio, now endemic in only four countries—Afghanistan, India, Pakistan and Nigeria.
“Even if they don’t come down with any symptoms (carriers), by giving them polio vaccine we make that person less infectious,” said Oliver Rosenbauer, WHO spokesman for the Global Polio Eradication Initiative in Geneva.
To treat rare disease, NIH scientists repurpose FDA-approved drug
|
|
WHAT: A new study reports that a drug already approved by the Food and Drug Administration for use in patients undergoing a bone marrow transplant may also have promise for treating people who have a rare immune deficiency known as WHIM syndrome. People with the syndrome are more susceptible to potentially life-threatening bacterial and viral infections, particularly human papillomavirus infections, which cause skin and genital warts and can lead to cancer. The study was conducted by investigators at the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health (NIH).
Boys and girls are equally at risk of inheriting the genetic mutation that causes WHIM syndrome, and the disorder frequently affects multiple family members. Approximately 60 patients worldwide have been diagnosed with WHIM syndrome, 10 of whom are currently receiving care at NIH.
As a result of the inherited genetic mutation, the function of a molecule, called CXC chemokine receptor 4 (CXCR4), increases. This in turn inhibits migration of neutrophils and other types of white blood cells from the bone marrow into the bloodstream. With fewer circulating immune cells, those with the disorder are less able to fight off infections.
New Gene Therapy Technique on Induced Pluripotent Stem Cells Holds Promise in Treating Immune System Disease
|
|
Researchers have developed an effective technique that uses gene therapy on stem cells to correct chronic granulomatous disease (CGD) in cell culture, which could eventually serve as a treatment for this rare, inherited immune disorder, according to a study published in Blood, the Journal of the American Society of Hematology.
CGD prevents neutrophils, a type of white blood cell of the immune system, from making hydrogen peroxide, an essential defense against life-threatening bacterial and fungal infections. Most cases of CGD are a result of a mutation on the X chromosome, a type of CGD that is called “X-linked” (X-CGD).
While antibiotics can treat infections caused by X-CGD, they do not cure the disease itself. Patients with X-CGD can be cured with a hematopoietic stem cell (HSC) transplant from healthy bone marrow; however, finding a compatible donor is difficult. Even with a suitable donor, patients are at risk of developing graft-versus-host disease (GVHD), a serious and often deadly post-transplant complication that occurs when newly transplanted donor cells recognize a recipient’s own cells as foreign and attack the patient’s body.
Smoking in combination with immunosuppression poses greater risk for transplant-related carcinoma
|
|
Spanish researchers have found that liver transplant recipients who quit smoking have a lower incidence of smoking-related malignancies (SRM) than patients who keep smoking. In fact, SRMs were identified in 13.5% of deceased patients and smoking was associated with a higher risk of malignancy in this study. Full findings are published in the April issue of Liver Transplantation, a journal of the American Association for the Study of Liver Diseases.
While smoking is a well-known malignancy risk factor both in the general population and in liver transplant recipients, smoking in combination with immunosuppression is presumed to be the main risk factor for transplant-related carcinomas. Several authors have suggested that a longer duration of immunosuppressive treatment or a stronger immunosuppression could be related to a higher risk of malignancy. However, the Spanish researchers failed to find such an association. Rather, they suggest that smoking after transplant which increases the risk, and smoking cessation following transplant surgery which decreases the risk, are more significant indicators.
“Smoking is related to some of the most frequent causes of post-transplant malignancy,” says study leader Dr. J. Ignacio Herrero of the Clínica Universidad de Navarra in Pamplona, Spain. “We investigated whether the risks of developing malignancies was different in patients who ceased smoking than in patients who maintained smoking after transplantation.” Risk factors of lung, head and neck, esophagus, kidney and urinary tract (other than prostate) cancers after liver transplantation were examined in the present study.





